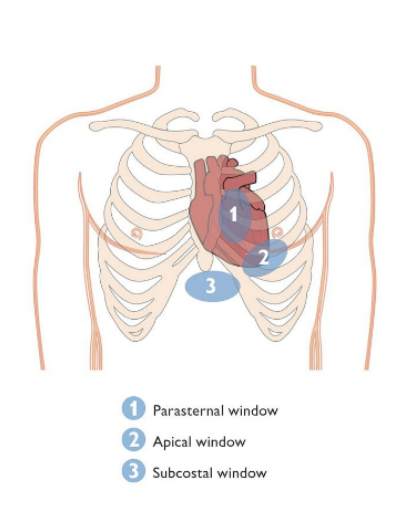
The presence or risk of cardiac tamponade.Treatment for pericardial effusion depends on: However, pericardial effusion may be diagnosed when these tests are done for other reasons. A chest X-ray can show signs of an enlarged heart if the effusion is large.ĬT and MRI scans can detect pericardial effusion, although they're generally not used to look for the condition. An X-ray image of the chest allows a health care provider to check the size and shape of the heart. Your cardiologist or another health care provider can look for signal patterns that suggest cardiac tamponade. Wires connect the electrodes to a computer, which displays the test results. Sticky patches (electrodes) are placed on the chest and sometimes the arms and legs. This quick and painless test measures the electrical activity of the heart. An echocardiogram may also show decreased heart function due to pressure on the heart (tamponade). The test can help determine the amount of fluid between the two layers of the pericardium. An echocardiogram shows the heart chambers and how well the heart is pumping blood.

Sound waves are used to create pictures of the heart in motion. Although the pericardial involvement of Henoch-Schonlein Purpura seen in this patient is rare, any collagen vascular disease can present with pericardial effusion and might respond to appropriate anti-inflammatory therapies including steroids if recognized promptly.Tests to diagnose or confirm pericardial effusion may include:
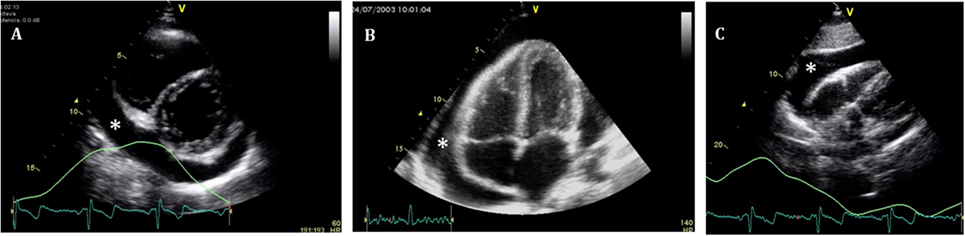
HSP presenting as pericardial disease has only been reported in a few cases. It rarely involves the myocardium or pericardium and is even rarer to present as a large pericardial effusion, especially in an adult.
#Trivial pericardial effusion skin
HSP is a rather common disease in children with systemic hypersensitivity vasculitis in the skin and other organs including the kidneys. It rarely presents with significant pericardial disease, especially in adults, and is a rare entity with only a few reported cases. It is characterized by a tetrad of palpable purpura, arthralgia, abdominal pain and renal disease. Henoch-Schonlein Purpura (HSP) is the most common form of systemic vasculitis in children. A repeat echocardiogram was obtained which showed only trivial pericardial effusion with no signs of tamponande. The patient was started on high dose steroids with marked improvement in his symptoms including a decreased pericardial effusion. Pericardial fluid was consistent with acute inflammation with several neutrophils but no growth on culture. Biopsy of the skin purpura was consistent with IgA leukocytoclastic vasculitis with intense deposition of IgA within the superficial dermal blood vessel walls. Laboratory evaluation revealed markedly elevated C-Reactive Protein of 225. He was found to have a large pericardial effusion on an echocardiogram with respiratory variation requiring drainage. Physical exam showed cardiac dullness beyond the apical point of maximal impulse, elbow joints with limited range of motion and swelling, periungal erythema and palpable purpura over his extremities.

A 49 year old Male presented with a two month history of progressive dyspnea, polyarthralgia, fatigue, and skin rash.
